When you first became a doctor, did you ever imagine you’d be taking your camera into work?
Not at all. I got into medical photography when I started my anaesthetics training at University College Hospital in London. It’s a dynamic place with lots of educational projects going on that need imagery. So I began by shooting in operating theatres, outpatients’ clinics and on the wards. I soon realised what a challenge taking photographs is in the clinical environment, and also how satisfying.
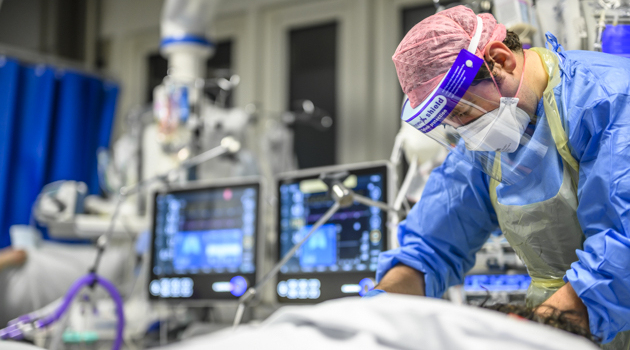
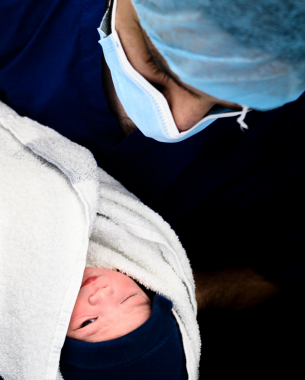
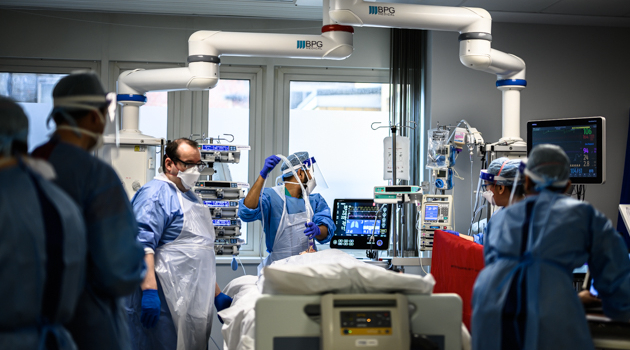
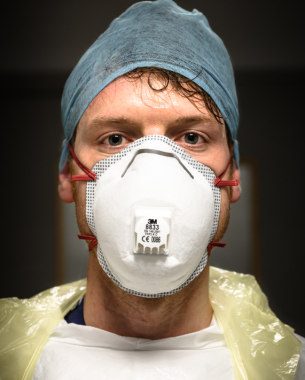
When the pandemic hit, I was in my current post at the Whittington Hospital in North London. My consultant supervisor, knowing I was a photographer, thought it would be a good idea for me to document what was happening. I’d had a similar thought, and we ended up approaching each other on the same day.
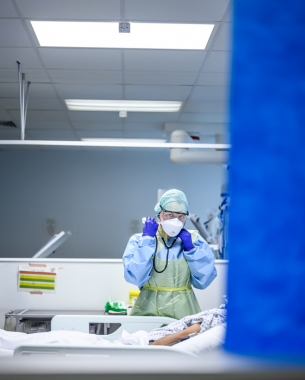
I started shooting in April 2020, using my Nikon Z 6 and the 24-70mm f/4 kit lens. Everything was handheld because a tripod would have got in the way, and was also a contamination risk – for the same reason, I didn’t even use the camera strap. I wanted to shoot in a raw, unstaged manner with available light – flash would have been too disruptive for the patients and staff. I wasn’t after studio-style, perfectly lit portraits; I wanted to show the processes, patient journeys and themes, to educate people about the pandemic and to document the medics’ stories, too.